By Sophie Holman-Jones, Third year, Biomedical Sciences
Last month, a paper by University of Bristol fellow Dr. Jessica Watson highlighted the inaccuracies of lateral flow testing, urging healthcare professionals to be more transparent with patients.
With over 3,500 new COVID-19 cases in Bristol in the last week alone, coronavirus still continues to remain a very prominent threat to our city. The scale of this threat means it is likely that you will have at some point taken a lateral flow device (LFD) test, which is intended to identify the virus in asymptomatic individuals.
LFD tests quickly search liquid samples to detect traces of the SARS-CoV2 antigen, a protein that is situated on the outside of the COVID-19 pathogen, and hence why these tests are also referred to as ‘rapid antigen tests’.
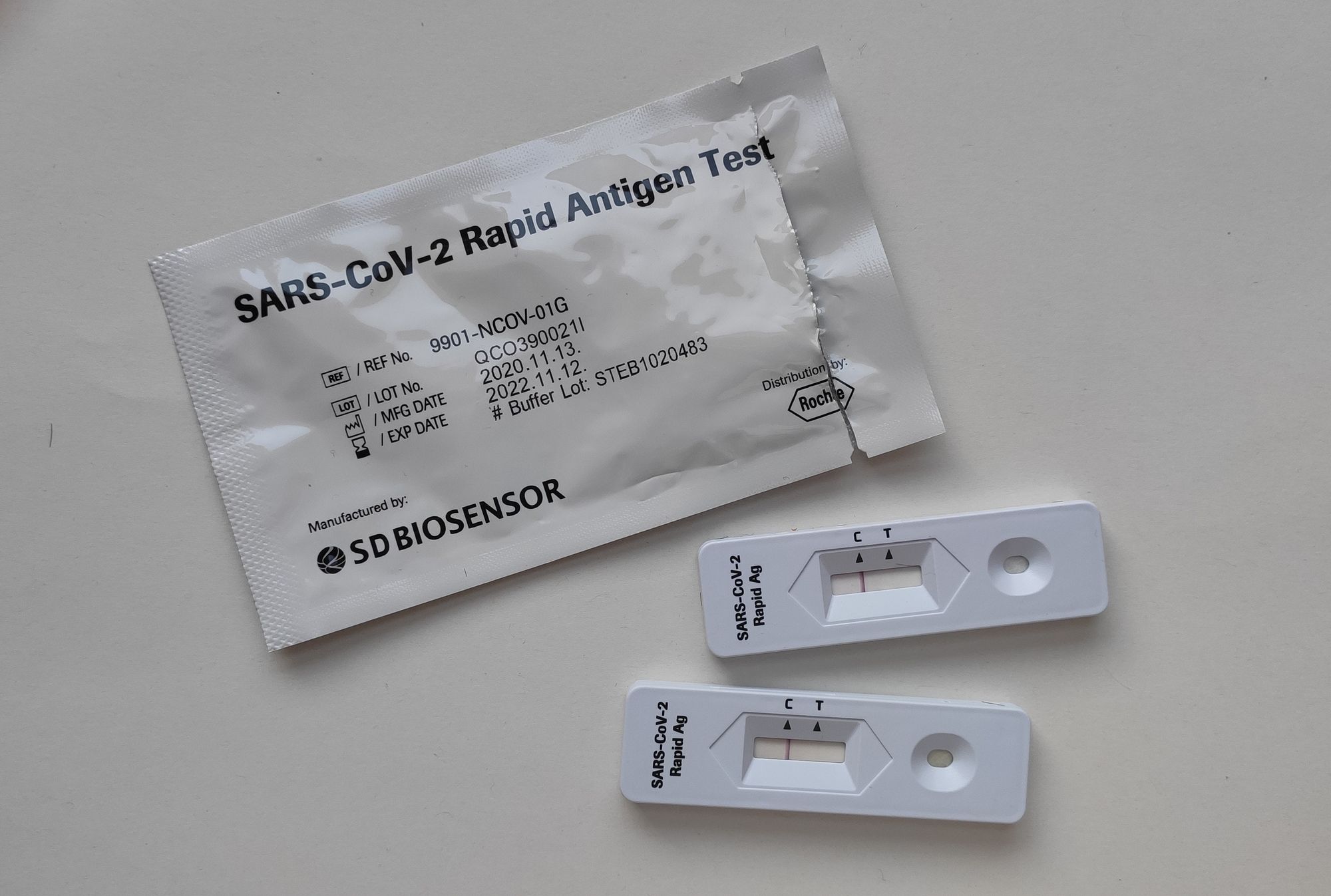
LFD tests are freely available in England to everyone over the age of eleven, and may be utilised on the basis of “test to enable” meaning pre-emptive testing before social events, or for “test to release”, as a way of determining whether ten-day isolation rules still need to remain in place for those who have been in contact with an infected person.
Unfortunately, LFD tests are unreliable, and in order to gain a conclusive result, a polymerase chain reaction or ‘PCR’ test should be arranged either at home or at a COVID testing centre within two days of receiving a positive result.
The lack of LFD reliability no doubt has damaging implications for various public sectors on a national scale. Firstly, the need for multiple tests in order to obtain a reliable result will be costly to governmental and NHS resources. In addition to the financial aspect, members of the public are exposed to an unnecessary risk either from contact with infected individuals at PCR test centres or in the street while travelling to PCR appointments.
LFD tests are unreliable, and in order to gain a conclusive result, a polymerase chain reaction or ‘PCR’ test should be arranged
Up to twelve days’ work could be missed by employees due to the wait for a PCR test, which, had a more conclusive test been used initially, would have been limited to only ten days. This demonstrates that the current LFD tests have costs to national productivity, which collectively amounts to a vast national debt. All of these implications could be avoided completely should LFD tests be accurate and definitive, but why is this not the case?
The efficacy of LFD tests is compared against PCR as a gold standard and assessed on the basis of test specificity and sensitivity to the virus. However, according to a paper published by the BMJ, these assessment parameters are limited and other factors should be considered when interpreting the result of an LFD test.
Co-author Dr. Jessica Watson, a GP and a NIHR Doctoral Research Fellow at the University of Bristol’s Centre for Academic Primary Care and Applied Research Collaboration (ARC) West, specialises in how GPs use diagnostic tests in primary care. Dr. Watson collaborated with researchers from the University of Cambridge and Trinity College Dublin on this work.

The team recommends that in order to give a more comprehensive and representative diagnosis of COVID-19, the ‘pre-test probability’ should also be considered by clinicians in addition to the test specificity and sensitivity. In other words, this probability is the likelihood of an individual contracting the virus depending on a range of health and life-style factors, such as local epidemiology, their vaccination status and whether the LFD test was performed correctly. Only after a holistic consideration of the context of each case can a test result be deemed reliable or unreliable.
Dr Watson has encouraged healthcare professionals to remain “open, share uncertainty, and [avoid] oversimplifying” with regards to the inaccuracies of LFD testing. This concept has shown to be effective in a recent trial, whereby incorporation of uncertainty around PCR testing resulted in fewer people feeling that their results were conclusive, and as a result taking a cautious reactive approach, for example continuing to self-isolate if they tested negative with symptoms.
Understanding the second wave: COVID-19 antibody testing in Bristol
The COVID-19 vaccine: busting the myths
Should this new advice be adopted, we could see a revised and revolutionised testing scheme in the near future, which could save governmental and NHS spending, further protect public health and increase national employment efficiency.
Featured image: Unsplash / Annie Spratt
Do you still feel uncertain after a negative result from a rapid antigen test?