By Will Smears, Fourth Year, Biochemistry
Somerset has among the worst incidences of injection drug-related deaths in the UK, with Bristol accounting for a large proportion of them. Opioid users often lack access to medication for opioid overdoses, but an app developed partly by University of Bristol researchers aims to solve this problem.
Opioids can be extracted from Papaver somniferum (Poppy plant) or synthetically developed. Codeine, morphine and fentanyl are opioids historically used for pain-relief, but are also used recreationally alongside other opioids such as heroin, oxycodone and methadone.
Opioids attach to opioid receptors in the brain and spinal cord, blocking the transmission of pain signals. They intensify triggering feelings of pleasure and sedation, by stimulating the release of endorphins (happy chemicals). Relaxation and sleepiness can be induced through slow breathing and a reduction in heart rate. In an overdose, this can cause breathing problems and unconsciousness, which is often fatal.

Opioid prescriptions in the UK more than doubled since 1998. This has been described as an ‘epidemic’. Many public health workers think that opioids are promiscuously prescribed, often in cases of chronic pain, for which they are of little use. Clinically prescribed opioids as well as illegal street opioids, such as heroin, have contributed to an increase in opioid-related deaths across the UK, despite an overall decrease in the rate of addicts.
The increase in mortality rates is largely attributed to an ageing cohort of drug users, with the highest rate of users among the 45-49 year age group. This may be due to the effects of long-term use making users more susceptible to overdose.
In 2021, 4,859 drug poisoning deaths were registered across England and Wales, with a rate of 84.4 deaths per million. The South West had a particularly alarming rate of 91.4 per million. Nearly half of all these deaths involved an opiate, a natural opioid. 49% of opioid users in Somerset did not access hospital treatment compared to the English average of 47%.
Injecting drug use is particularly prevalent in Bristol, an epicentre for ‘snowballing’ – injecting a mixture of crack cocaine and heroin.
The statistics clearly show a need for improved medical assistance for opioid users in Somerset, which the ‘Carry Naloxone’ app aims to help fulfil. The app was partly developed by researchers at the University of Bristol, and encourages opioid users to carry naloxone, a medication to treat opioid overdoses.
Naloxone is an opioid antagonist. It effectively ‘kicks off’ opioids from opioid receptors and blocks them from generating further effect. Naloxone is extremely effective; either the nasal spray or injection can restore normal breathing within two minutes.
On entering the app, there are several tabs providing information resources. The first outlines the symptoms of opioid overdose, and instructions on administering naloxone. It also tells users how to reduce the risk of overdose. With location access, the app can show a map with the locations of pharmacies stocking naloxone.
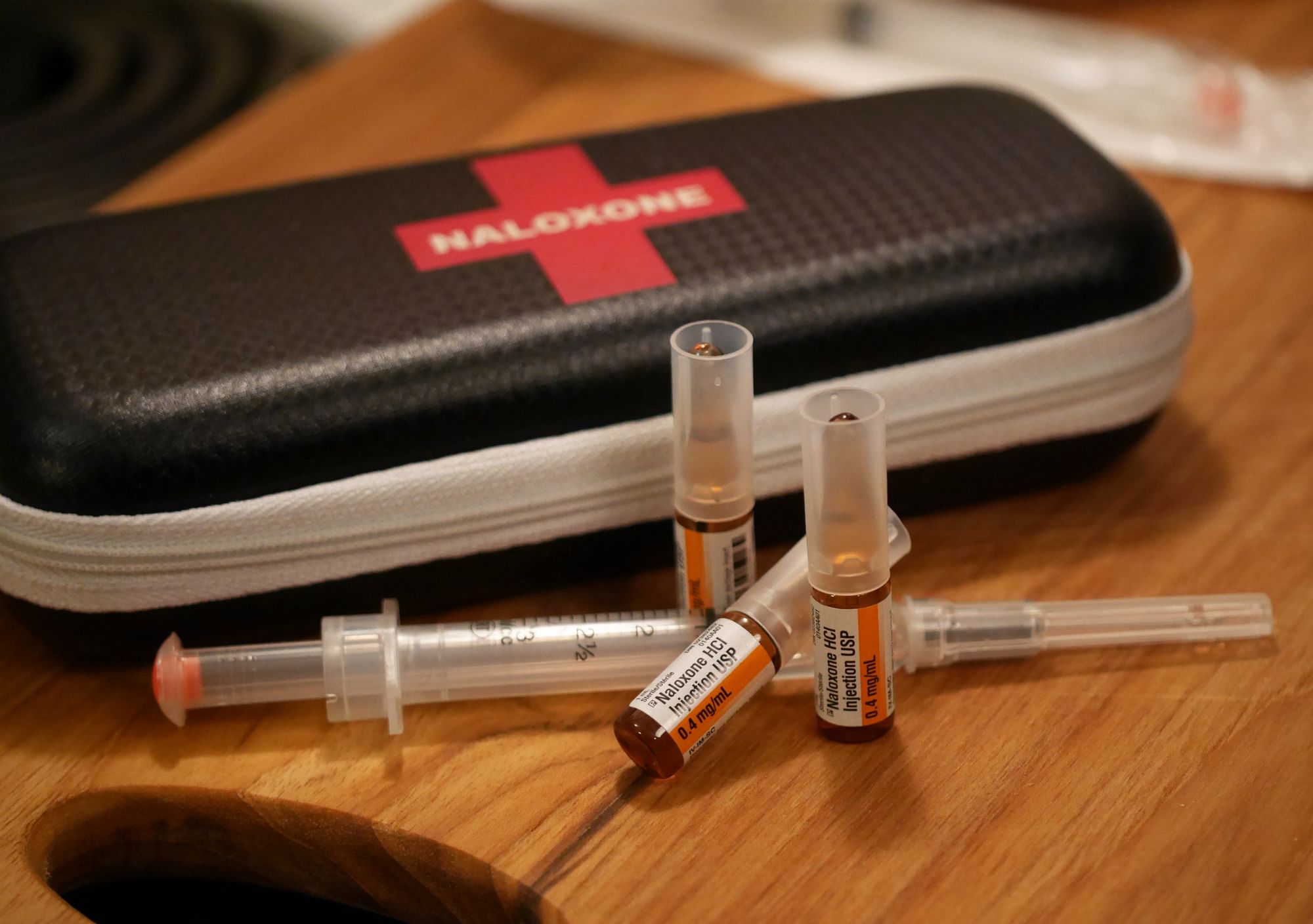
Drs Jennifer Scott and Jo Kesten from University of Bristol Medical School, alongside Deb Hussey from Turning Point UK, performed surveys and workshops with victims of overdose, witnesses to overdose, current users and drug service staff. Dr Scott hopes that the app will be more ‘engaging’ information material to ‘help raise awareness of naloxone and where to get it and encourage people in Somerset to carry naloxone’.
The app was written by University of Bath computer science student Tom Heaton. Somerset Council funded the project to support the 2021 ‘From Harm to Hope’ Government drug strategy, a ten-year plan that aims to reduce drug-related deaths across the UK.
‘Naloxone should be seen as an essential medication and thought of in the same way as a defibrillator, or an EpiPen for anaphylactic shock,’ says Adam Dance, Lead Member for Public Health, Equalities and Diversity at Somerset Council. ‘I did the training last year. It’s easy to administer, easy to carry and can ultimately save someone’s life’.
There is still a long way to go before the end of the opioid epidemic, but this app may be a big step towards reducing mortality rates among opioid users in Somerset.
Featured image: Unsplash / Jonathan Gonzalez
Will you be downloading the 'Carry Naloxone' app?









