Last summer, sat between my parents and a few too many glasses of wine, I listened as they argued over whether magic mushrooms could remedy depression and even boost the odds of recovery from chemotherapy. My mum, a firm believer in the mind’s power over the body, was adamant that microdosing psychedelics could improve mental and, in turn, physical health. My dad, defending orthodox medicine, scoffed at the notion that shrooms could ‘cure cancer’. As a biochemistry student, my desire was to side with biomedical science, however, as a woman my instinct drew me to my mother’s conviction in the strength of a magic mushroom-based cure.

The unconventional approach my mum was defending is a type of complementary and alternative medicine (CAM), a loose collection of practices that fall outside mainstream healthcare. CAM is widely regarded as holistic, treating the individual’s physical and psychological experience of illness, rather than the disease itself. Think acupuncture, herbal remedies, and traditional Chinese medicine, among many others. Complementary therapies are used alongside conventional medicine, while alternative therapies are used in place of traditional care.
Women are consistently more likely to use CAM than men, a difference in attitudes that may well stem from a feeling of being sidelined by traditional medicine. Throughout history, female anatomy has been misunderstood, feared and pathologised. In ancient Greece, physicians claimed the hystera (womb) could wander throughout the body and press on organs, causing irrational behaviour and physical illness, a diagnosis they called ‘hysteria’.
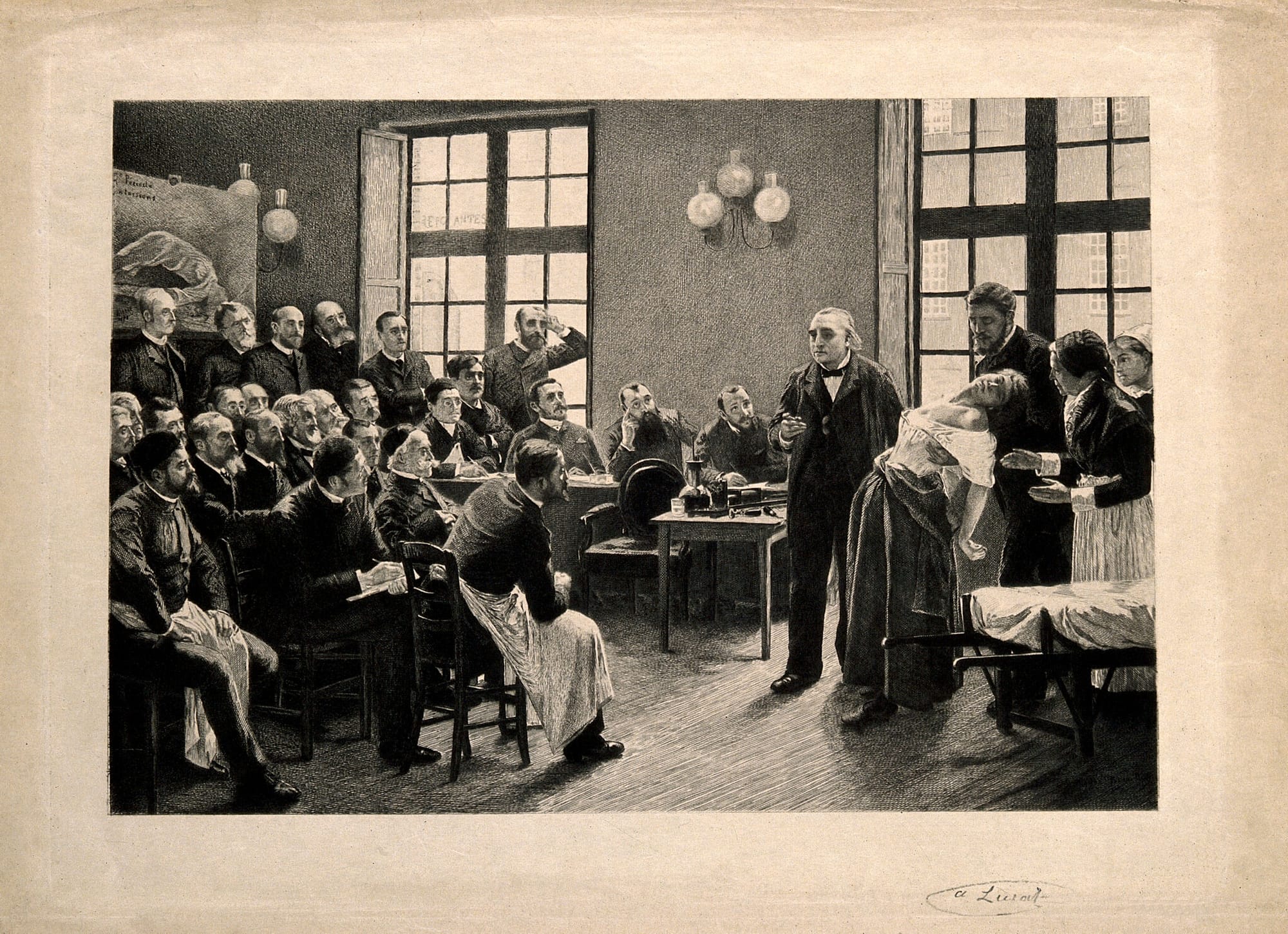
For centuries, female sex organs provided the explanatory source of almost any disorder, from depression to kleptomania. Some physicians thought a build up of sexual fluids and menstrual blood incited lascivious behaviour in women. The solution sought to expel this corrupting fluid: married women were prescribed regular intercourse with husbands, whose semen allegedly wielded healing properties, while unmarried patients were ‘treated’ by midwives. This logic continued into the 17th century in the guise of the ‘uterine massage’, in which trained professionals stimulated female patients to a ‘paroxysmal convulsion’. In plain English, the cure for nymphomania and other, conveniently, feminine disorders was a doctor-ordered orgasm.
Black women, in Antebellum South, faced gross mistreatment in the realm of mainstream gynaecological practices. Physician J. Marian Sims famously found the cure to fistulas (an abnormal internal opening arising post-childbirth that causes debilitating incontinence) through his brutal and relentless experimentation of enslaved women. Convinced Black women had a naturally higher tolerance for pain than White patients, Sims refused to administer anaesthesia whilst operating. Sim’s pioneering surgeries earned him the title ‘father of gynaecology’, a status built on the exploitation of black women. Yet misogyny in medicine, and its intersection with racism, did not end with Sims. In the UK, as recently as the mid 2010s, studies found that black women were around five times more likely than white women to die from pregnancy and childbirth complications.
Today, the ongoing neglect of women in healthcare is often referred to as the Gender Pain Gap. The term describes the social phenomenon in which women’s pain is still taken less seriously than men’s, leading to longer diagnostic delays and the need for multiple GP appointments before being referred for conditions like heavy periods and endometriosis. These repeated invalidations have led some women to stop seeking further care after feeling unheard, highlighting a dangerous social flaw in which serious conditions may go untreated, and women’s health and wellbeing are placed at significant risk.
Beyond the everyday dismissals, there also exists a fundamental lack of research into women’s health therefore doctors may not be equipped to recognise female specific symptoms to begin with. Women make up more than half the country’s population, yet only two per cent of medical funding in the UK is directed to maternal and reproductive female health, and for decades men were the default in clinical trials. Take heart disease, the leading cause of death in both men and women, yet heart attacks in women are still more likely to be missed or mismanaged. Even when presenting with typical chest pain, doctors are often working within male-oriented models, so women are diagnosed later, prescribed less aggressive treatment and are around three times more likely to die as a result.
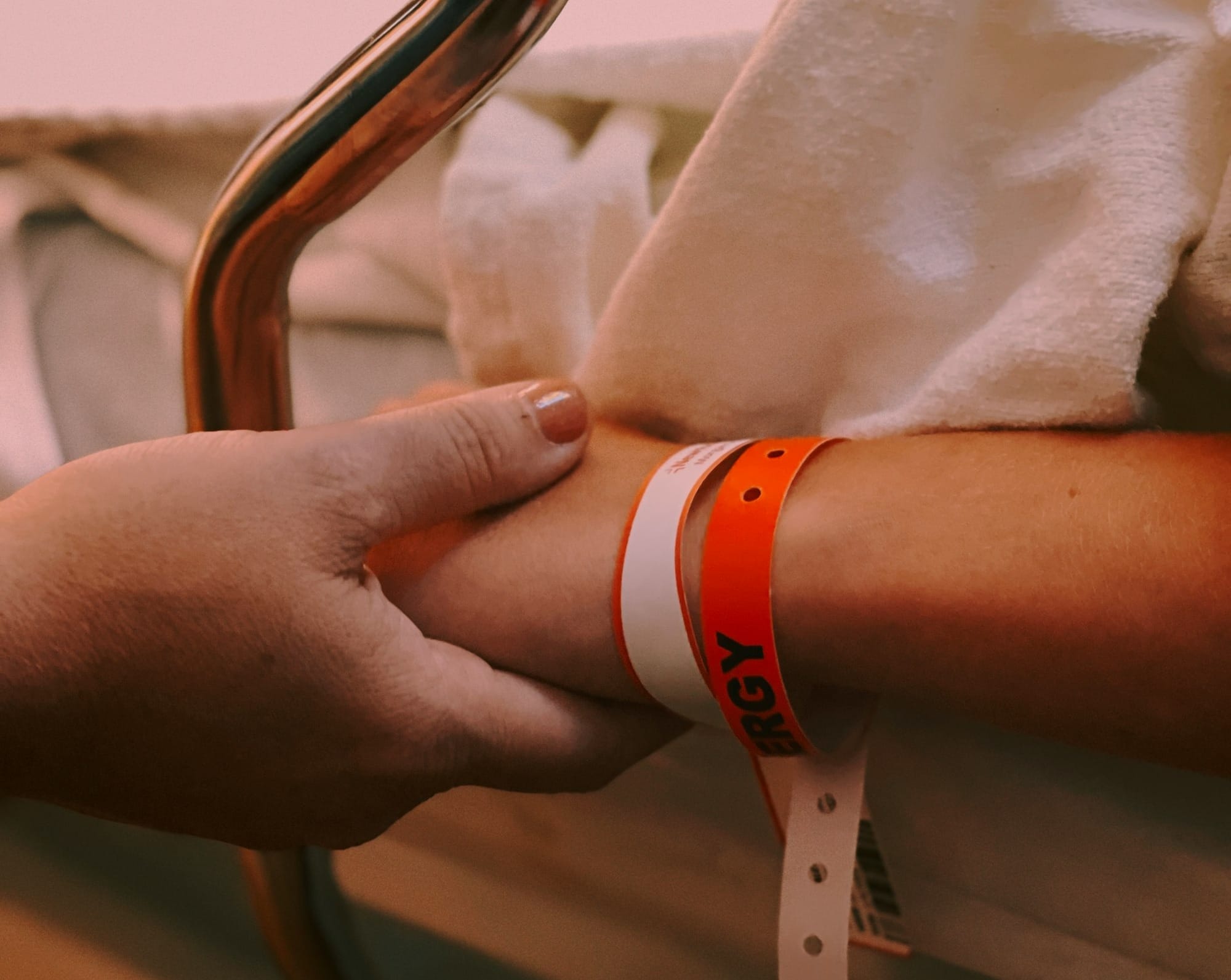

When medicine has long treated women’s bodies as expendable and their concerns as dismissible, it is hardly surprising that many look for alternative care. While the effectiveness of CAM is questioned by scientists (and my dad), a 2023 review cites clinical hypnosis as a viable alternative to hormone therapy for menopausal hot flashes and night sweats. When women are not compatible with mainstream treatment, whether due to complicating health conditions or personal preference, CAM can offer a different avenue that seeks to treat the whole lived experience of illness and do so without judgement.
That is not to say that a cup of green tea rivals a GP appointment, but the attitude among many, that CAM is a fraudulent or completely ineffectual practice is harmful and may stop doctors from recommending, potentially helpful, options to women who are not fit for traditional treatments. Neither a single social nor personal factor can determine the reason women turn to CAM. From ancient society to present day, mainstream medicine has repeatedly failed to listen, represent, and treat women equally, thus the search for unorthodox care becomes less laughable and a more necessary means of survival.
Featured Illustration: Epigram / Tess Rayner
What do you think could be done to close the Gender Pain Gap?