By Luke Beaumont, First year, Psychology and Neuroscience
It starts with a little itch. Not an unusual one. Not painful, not alarming, an easily forgettable sensation. The kind you would normally scratch without thinking. Except this time, there is nothing you can scratch. The hand is gone.
Phantom limb syndrome describes the experience of feeling sensations in a limb that has been amputated. These sensations can be subtle - a slight tingle, a warmth or even a movement - or a harrowing, intense pain. Remarkably, up to 80 per cent of amputees report some form of phantom sensation. The body part is absent, but the experience of it persists.
This raises an important question which sits in the centre of neuroscience: if sensation comes from the body, how can sensation exist without it?
The answer lies not in the missing limb but instead the deep and remarkable structure of your cortex.
The brain’s map of the body
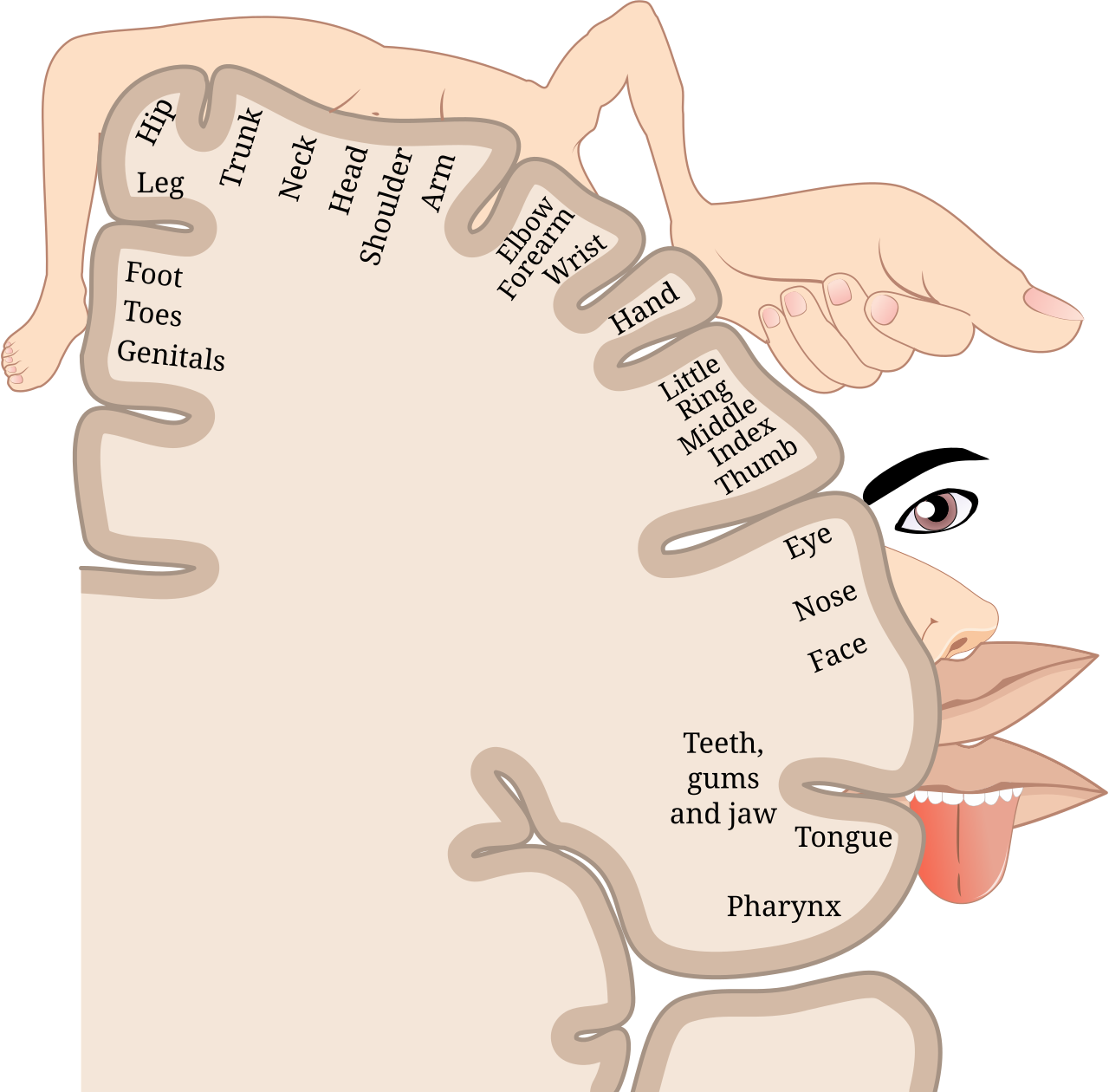
First, we must consider the pathway from limb to brain. Our limbs are full of sensory neurons responsible for everything from the textures we feel to even the position of our body in space, known as proprioception. Neural pathways carry this sensory input up to the brain. At the core of this phenomenon is the somatosensory cortex, a large region responsible for processing bodily sensations. This area by nature is organised in a precise, cartographic way - different regions correspond to different parts of the body, forming what is referred to as the ‘sensory homunculus’. The hand, the face and the foot each has its own place on the cortex.
When a limb is lost, its corresponding region in the brain does not simply get ‘turned off’, it remains active, still capable of generating sensations. Thus, the brain, in effect, continues to believe the limb still exists.
Over time, this map begins to change. Through a process known as neuroplasticity, neighbouring regions start to expand into the now-unused space in the cortex. Now, blurring the boundaries of the body map. In some cases, this produces strange effects touching a patient’s face can elicit sensations in a phantoms hand because the facial and hand representations lie adjacent in the cortex.
The body is no longer a direct reflection of physical reality. It is a reconstruction - subjective, dynamic and occasionally inaccurate.
When the sensation becomes pain
For many sufferers, phantom sensations are not a curiosity - they are painful.
Phantom limb pain can take many forms: burning, cramping, even a feeling of being stabbed. Some patients report that their phantom limb feels frozen in an uncomfortable position, unable to move. This introduces a deeper layer to the problem. The brain is not only maintaining the somatotopic representation of the limb, but also the memory of how it felt.
There are two leading explanations. The first centres on a mismatch between motor intention and sensory feedback. When the brain sends a command to move the missing limb, it receives no confirming sensory input in return. This unresolved loop may contribute to the persistence of pain, as the brain attempts to reconcile conflicting information. In this sense, phantom pain is not simply a lingering echo of the body, it is an active, ongoing construction.
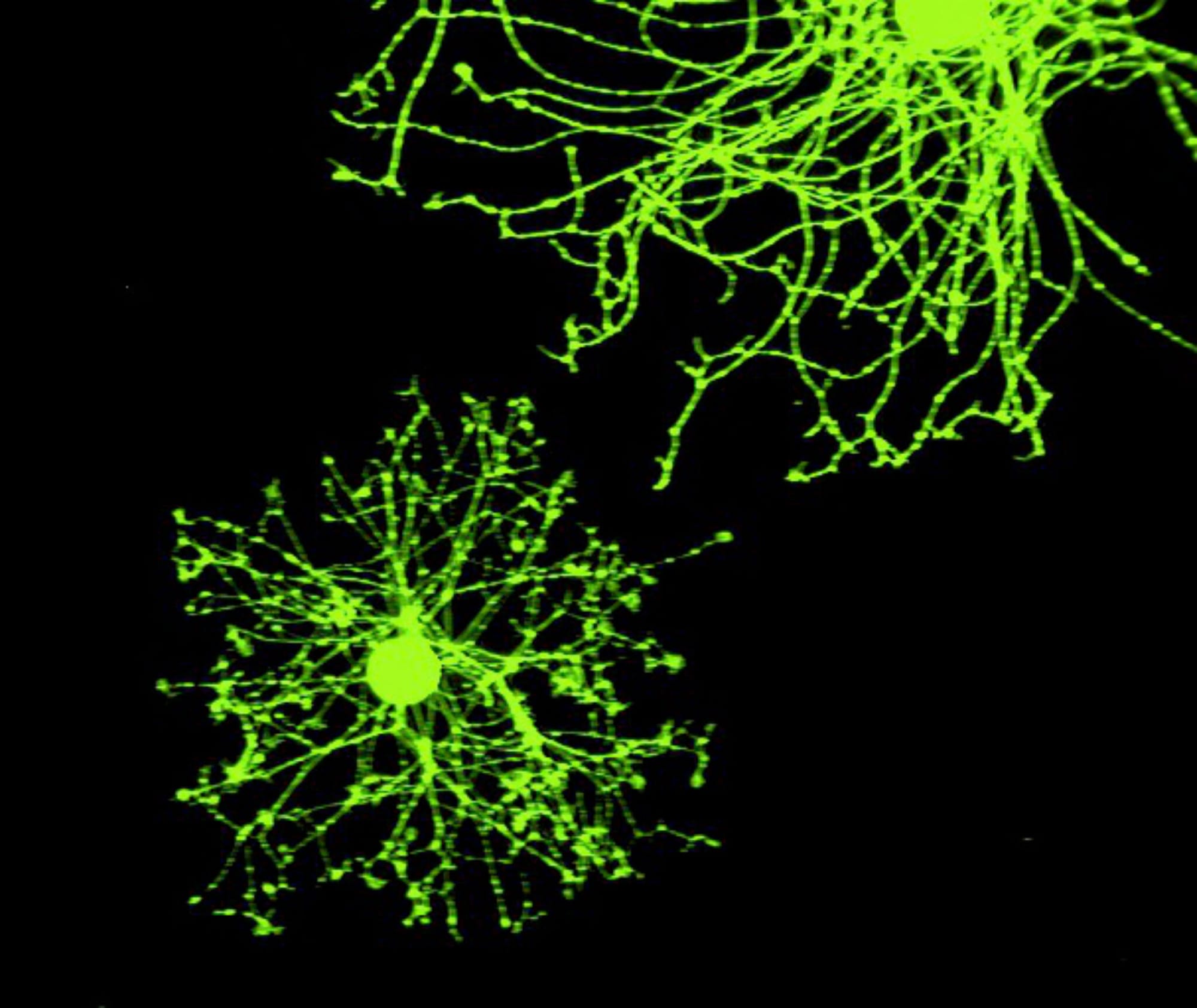
The second explanation is far more grounded in neuroscience. Neurons exist in dense networks, constantly receiving input from neighbouring cells through synapses. These synaptic connections are not fixed, when input is lost, the synapses begin to weaken and retract (known as synaptic pruning) - particular at their outermost branches. After amputation, neurons that once received signals from the limb fall silent. But they do not stay inactive for long, nearby neurons begin to extend into this inactive space, and the boundaries between adjacent sensory neurons begin to blur. As a result, the signals from one part of the body can spontaneously activate areas which once belonged to the missing limb. The brain (still relying on its existing somatotopic map) interprets this activity as a sensation from the amputated body part.
Therefore, phantom pain is not coming from the limb itself, but from a system trying to erratically reorganise itself after losing input.
Tricking the brain: Rewiring the circuit
One of the most compelling treatments for phantom limb pain comes from the work of V. S. Ramachandran, known as mirror therapy.
A mirror is placed between the limbs so that the reflection of the intact limb appears where the missing limb would be. When the patient moves both limbs (e.g. their hands) simultaneously, the brain ‘sees’ the absent limb moving. This simple illusion provides the visual input the brain has been missing, helping to reduce pain.
But treatment doesn’t just stop there. Because phantom pain is partly driven by neighbouring neurons expanding into inactive areas, therapies also aim to stabilise these changes. Repeated visual feedback (often using the mirror box), sensory training and even techniques like virtual reality help reinforce more accurate body maps, limiting the spread of neighbouring activity.
Rather than repairing the body, these approaches attempt to reshape the brain cortex - guiding it back to a more stable representation of itself.

A body predicted, not perceived
Phantom limb syndrome reveals something much deeper than a neurological curiosity, the brain does not simply register the sensations of the body - it predicts it. Even after amputation, the motor cortex continues to send commands to move the missing limb, while the brain maintains expectations of how it should feel. With no absent sensory input to correct these signals, the system begins to rely on its own internal map.
Studies showing the effectiveness of treatments like mirror therapy highlight just how flexible the system is and how easily perception can be distorted when the brain is given new input. Thus, phantom limbs are not errors but are consequences of a system designed to anticipate and adapt.
The body we experience is not a direct reflection of reality; but the product of prediction, plasticity and perception - all working together to provide our subjective reality.
Featured Image: Unsplash / ThisisEngineering
Do you know anyone affected by phantom limb pain?










